Is there a more innocuous seasoning in your kitchen than salt? As the most common condiment in cooking, it’s easy to sprinkle into your dinner without thought. From our modern perspective, it is hard to imagine how important salt has been throughout human history. Empires have risen and fallen from its trade. Gandhi’s civil resistance for Indian independence centred around the Salt March, a protest on a salt tax imposed by the British Empire. And that’s because salt isn’t just mild seasoning, it’s one of our five basics tastes and an essential mineral for life.
There are many physiological and cellular functions that depend on salt. Salt is vital for homeostasis, which is the regulation of physical and chemical conditions in the body, constantly being rebalanced by feedback loops. Specifically, salt is vital for regulating water. Salt is also required for specialised functions in regulating blood volume and pressure, as well as enabling the conduction of nerve signals.

Unfortunately, though, sources of salt are hard to find in nature. The oceans that provide rain through water vapour leave the salt behind during evaporation. Geological sources are incredibly rare, and become harder to find the further you venture inland. Consequently, this lack of seasoning permeates throughout the food web. Plants have very little salt to extract and can’t serve salt to the herbivores that lie above them in the food chain.
And the high value of salt isn’t just a phenomenon of human society, it’s conserved in the selection pressures of evolution. Animals are driven to take high risk and energy intensive hunting for salty meat, as the opportunity for salty foods is irresistible to predators. But why do humans and animals have such a drive to find salty food?
This was the first study directly proving the powerful role of naturally released opioid neurotransmitters within the CeA in driving mammalian salt consumption.
Opioids and ‘MOR’ signalling in salt consumption
It’s a neuronal mechanism which has developed due to an intense evolutionary pressure for animals to crave and find salt.
It’s well known that opioids drive our “liking” (its palatability) and “wanting” (desire to consume) for salt. Opioids are neurotransmitters synthesised by the body which induce our appetite for, and encourage motivation to acquire food. Depending on how hungry a person is, and even their memory of the food, opioid-based neuronal signalling influences the tastiness of food. Many students will have a type of alcohol they can no longer drink due to a messy night out; you can blame that on your opioid signalling.
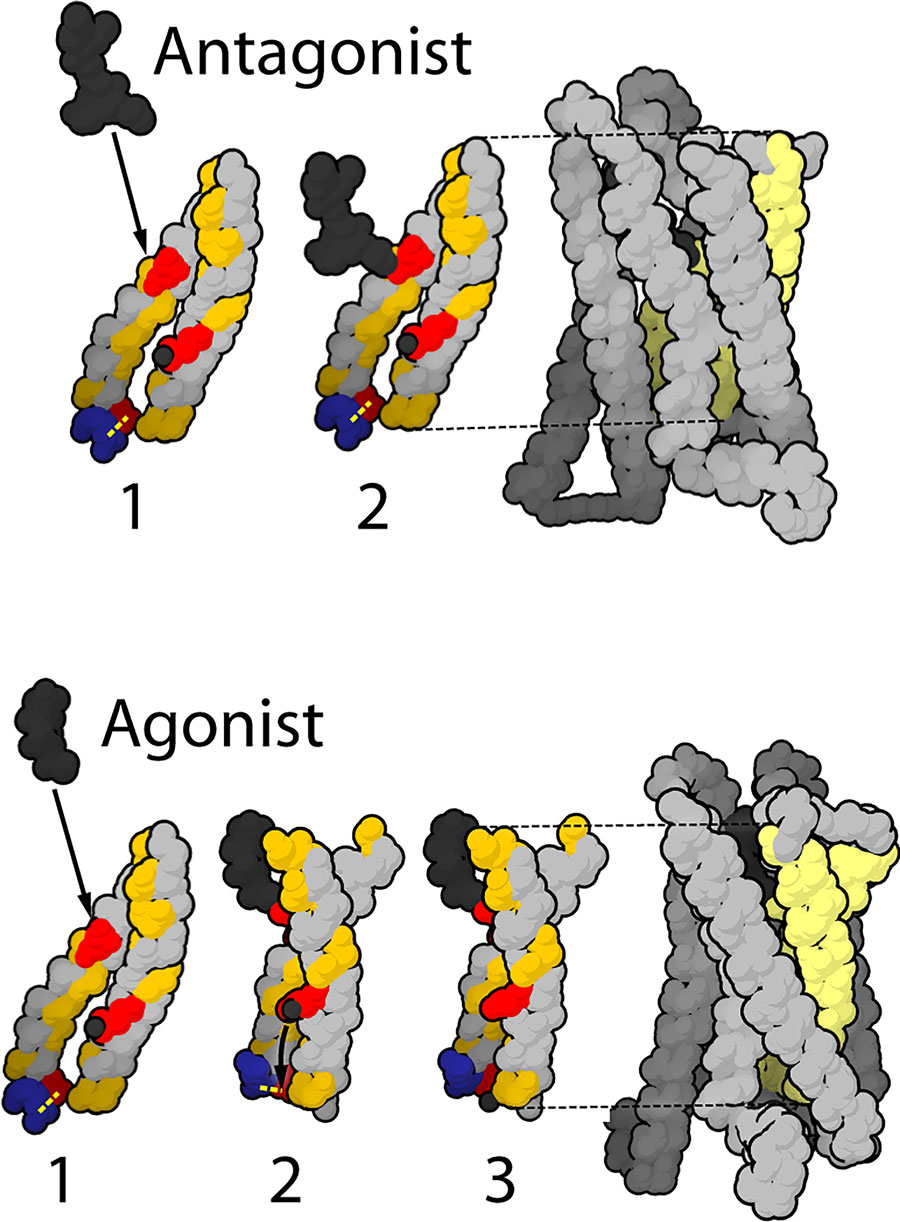
However, many of the finer details have long eluded scientists. What area(s) of the brain does this signalling take place in? What subtypes of receptors are used in the signalling pathway?
With help from collaborators, Dr Craig Smith at Deakin University has conducted research elucidating the neuronal mechanisms that help to drive our salt lust. Their experiments required them to feed mice low salt diets to control their salt intake with a single source of salt: a salty water solution. Mice are the ideal model organism for these experiments, as they have a similar brain structure to humans, including the same pathway for salt appetite.
Their first experiment used drugs to block subtypes of receptors for opioid neurotransmitters. Results identified the ‘mu opioid receptor (MOR)’ – a receptor which sends a signal when it binds with an opioid neurotransmitter – reduced the volume of salt consumed by more than half when it was blocked. That provides an answer for the receptor subtypes.
The central amygdala
But it doesn’t tell us anything about the location of the signalling. MORs are ubiquitous throughout the brain, and the experiment showed activity within numerous different sections of the brain. But their presence alone doesn’t give us any coordinates for their location.
Using immunohistochemistry, Dr Craig Smith identified the location. Immunohistochemistry uses antibodies which have receptors that bind to antigens, a protein sequence that complements the antibodies, allowing the antibody and antigen to bind. These antibodies can be developed to bind to any antigen, including a protein called ‘Fos’ that accumulates in neurons that have become highly active. When they bind, there’s an enzyme attached to the antibody which is activated and stains the antigen and its target cell. The target protein is now stained, and easy to see under a microscope.

Immunohistochemistry analyses found an increase in Fos from neurons in the central amygdala (CeA), showing that they became highly active while salt was being consumed. The CeA is a section of the amygdala that controls many innate and conditioned behaviours, including appetite-related and feeding behaviour. More importantly, this activity was curtailed by the MOR-blocking drugs, showing that the MOR receptors and their opioids are essential to the salt appetite for mice.
Building on these findings, Dr Craig Smith conducted another experiment where MOR-blockers were injected directly into the CeA section of the brain to test their effects. As one would expect from their previous experiments, the mice drank less from the salty water, despite still being placed on their low salt diet. This was the first study directly proving the powerful role of naturally released opioid neurotransmitters within the CeA in driving mammalian salt consumption.
The CeA is essential to this signalling using information from the senses. External senses such as the smell of salty snacks work in combination with homeostatic mechanisms which detect the body’s level of salt around the body. This combination triggers the neural signals to induce salt cravings. This is similar to the mechanisms used to drive general food cravings and conserved amongst mammals, from humans, to mice, and to Pavlov’s drooling dogs.
These results are significant in a modern society which has allowed humans to indulge, and overindulge, on salt for the first time in its evolutionary history.
Another follow up study was conducted to identify the particular neurotransmitters involved in CeA salt craving signalling. By using immunohistochemistry and different fluorescent markers for suspected neurotransmitters, Dr Smith discovered the culprits were enkephalin and calretinin. These neurotransmitters likely act both upstream and downstream of MORs within the CeA, and together, form a neurochemical chain reaction that drives salt consumption.
An opioid-salt addiction?
Attentive readers may recognise the word ‘opioid’ from a completely different context. As it turns out, the opioid pathways in our brain are connected to the opioid drugs that are the centre of the opioid epidemic in the United States of America. Opioid drugs work by hijacking our body’s many naturally occurring opioid receptor pathways, causing pain relief as well as addiction. As these pathways also control our response to salt, Dr Smith began to wonder if opioid drug use also affected the users’ response to salt.

This follow on experiment compared a non-opioid control with two other groups: people currently taking opioids and people who had been ‘abstinent’ (sober), for about one year. Results showed that the abstinent group had a greater palatability and craving for highly salted drinks than the other two groups. They were also the only group to continuously increase their desire for salted drinks as the salt concentration increased. This shows that the sensitivity that abstinent people continue to have towards opioids even after quitting (the basis for potential relapse) develops a “cross-sensitivity” with salt. This may be due to high concentrations of salt triggering the release of opioids, mimicking the impact of opioid drugs in the CeA.
These results are significant in a modern society which has allowed humans to indulge, and overindulge, on salt for the first time in its evolutionary history. What was once a scarcity – sometimes as highly valued as gold – can now be bought in large bags at our convenience. We can order meals saturated in salt within minutes to satiate our out-of-date desire for salt.
Our salt cravings are leading to hypertension, which increases the risk of suffering strokes, and kidney/heart diseases. According to the WHO, 1.13 billion adults worldwide had hypertension in 2015. The salt induced health crisis has never been worse for humanity.
Dr Craig Smith hopes that now their research has helped identify the neuronal pathways that underpin our drive for salt, it could be used to design drugs that block opioid receptors that are specific to these signalling pathways, thus targeting our neurons at the heart of our vice. This will undoubtedly be a valuable tool in a new fight, as societies are no longer fighting for more salt. For the first time in our history, we are instead battling our own inner desires to overconsume this once precious commodity.
Do your findings show that people taking opioids are more likely to suffer from diseases related to high salt, and should steps be taken to deal with this problem?
Our findings suggest that links between opioid use and salt-related diseases are plausible, and further work to investigate this would be important given the extent of the opioid epidemic. More directly however, our findings are more likely to help develop drug or psychological/behavioural strategies to reduce consumption of highly salted diet options like junk-food.
Could this research be used to help people with opioid addiction?
Eventually, this research could help recovering addicts to consume healthier diets with less salt and junk-food. However, the largest groups of people that this research is most likely to benefit are those with salt diet-induced hypertension that may lead to stroke or heart/kidney disease. Furthermore, this research may help individuals with obesity, type 2 diabetes, and other metabolic disorders that are caused by the overconsumption of highly salted junk-foods.
References
- Smith C, et al. (2016). Endogenous central amygdala mu-opioid receptor signaling promotes sodium appetite in mice. PNAS, 113 (48), 13893-13898.
- Smith C, Lawrence A. (2018). Salt Appetite, and the Influence of Opioids. Neurochem Res, 43, 12-18.
- Smith C, et al. (2019). Phenotyping neurons activated in the mouse brain during restoration of salt debt. J Chem Neuroanat, 101, 101665.
- Smith C, et al. (2019). The influence of opioid dependence on salt consumption and related psychological parameters in mice and humans. Drug & Alcohol Dependence, 203, 19-26.
- WHO, The (2019). Hypertension. [online] World Health Organization. Available at: https://www.who.int/news-room/fact-sheets/detail/hypertension [Accessed 08/01/2021].
10.26904/RF-134-102105
Funding
NHMRC (Australia)
Collaborators
Prof Andrew Lawrence, Florey Institute of Neuroscience and Mental Health
Bio
 Dr Smith is a Senior Lecturer and Laboratory Head at Deakin University, within the School of Medicine and IMPACT (Institute for Mental and Physical Health and Clinical Translation). His work investigates the neuronal pathways that control salt intake, feeding and stress, with a focus on peptides including opioids and relaxin-3.
Dr Smith is a Senior Lecturer and Laboratory Head at Deakin University, within the School of Medicine and IMPACT (Institute for Mental and Physical Health and Clinical Translation). His work investigates the neuronal pathways that control salt intake, feeding and stress, with a focus on peptides including opioids and relaxin-3.
 Professor Andrew J. Lawrence is an NHMRC Principal Research Fellow & Division Head at the Florey Institute of Neuroscience & Mental Health where he is leader of the Mental Health Research Theme and runs the Addiction Neuroscience laboratory. He is Editor-in-Chief of the Journal of Neurochemistry.
Professor Andrew J. Lawrence is an NHMRC Principal Research Fellow & Division Head at the Florey Institute of Neuroscience & Mental Health where he is leader of the Mental Health Research Theme and runs the Addiction Neuroscience laboratory. He is Editor-in-Chief of the Journal of Neurochemistry.
Contact

Dr Craig Smith
E: craig.smith@deakin.edu.au
T: +61 3 524 79473
W: https://www.deakin.edu.au/about-deakin/people/craig-smith
Prof Andrew J. Lawrence
E: andrew.lawrence@florey.edu.au
W: https://florey.edu.au/science-research/scientist-directory/professor-andrew-lawrence









