Professor Wang of the department of pathology and laboratory medicine and Professor Shi of the department of surgery at Children’s Hospital Los Angeles and the Keck School of Medicine of the University of Southern California have been investigating paediatric pulmonary disorders. Their research on alveolar capillary dysplasia with misalignment of pulmonary veins provides new evidence for diagnosing atypical presentations. The researchers have also uncovered previously unknown molecular and cellular changes present in congenital pulmonary airway malformation, and provide a new research direction for pathogenesis of this mysterious condition in children.
Aberrant lung development of an unborn foetus can contribute to several conditions that affect the quality of life and life expectancy of the individual. One such condition is called Alveolar Capillary Dysplasia with Misalignment of Pulmonary Veins (ACD/MPV). ACD/MPV is a rare but fatal lung disease that affects neonatal infants (infants in their first 28 days of life). ACD/MPV is an interstitial lung disease which affects blood vessels and surrounding pulmonary tissue, and is characterised by decreased capillary density, poor capillary-alveolar apposition, pulmonary septal thickening, and presence of misaligned pulmonary veins within bronchiovascular bundles, which cause breathing difficulties. There has been an excess of 200 reports of ACD/MPV since it was discovered in 1981. Most cases of ACD/MPV are sporadic (not familially inherited but arising from a gene mutation) but approximately 10% of cases are heritable.

Typical vs atypical ACD/MPV
ACD/MPV can be divided into two groups depending on the presentation of the disease: typical and atypical. Typical presentation will display symptoms such as progressive hypoxemic respiratory failure (a lack of oxygen in the blood that gets worse over time) and severe refractory pulmonary hypertension (abnormally high blood pressure in the arteries that carry blood to the lungs, which is unresponsive to treatment). Patients with typical presentation show symptoms within the first few hours of birth and do not survive beyond 28 days. Atypical presentation demonstrates a slower onset of symptoms (24+ hours, post birth) and/or survival beyond the neonatal period, which opens up avenues of potentially lifesaving treatments such as lung transplantation. Mutations of the FOXF1 gene have been identified in ~60% of patients suffering with ACD/MPV. However, presence of the FOXF1 mutation has been shown not to be a reliable indicator of typical or atypical cases, and pathologic features may be more useful for diagnosis and prognosis of typical/atypical ACD/MPV.
“This research represents a crucial advancement in the understanding of a deadly and mysterious paediatric lung disease. “
Classic vs non-classic morphologic features
In a recent study, Professor Larry Wang and Professor Wei Shi at the University of Southern California took a closer look at ACD/MPV. They divided ACD/MPV cases into ‘classic’ (characterised by an uniform diseased tissue which lacks of healthy capillaries within the lungs) or ‘non-classic’ (healthy capillaries present between diseased tissue). In their research, ten cases were ‘classic’. Classic cases showed underdeveloped lung lobules and abnormal blood vessel arrangement within the lung. The remaining six cases had a range of results. All cases had a mixed distribution of healthy-appearing lung tissue and abnormal lung tissue. Among them, one case had 50% normal lung tissue, whilst still displaying extensively abnormal pulmonary veins in 50% of the lung. This participant survived the longest of all participants in the study (254 days), implying perhaps unsurprisingly, that the larger amount of healthy lung tissue the participant had, the longer they survived.

Open lung biopsy: A lifesaving diagnostic indicator
The majority of ACD/MPV cases are diagnosed by post-mortem examination (autopsy). However, an earlier study demonstrated that 85% of diagnoses can be made using an open lung biopsy on a living patient. Importantly, the results of Wang and Shi’s detailed histopathological study suggests that the presence of misaligned alveolar veins (small veins in the air sacs of the lungs that fail to develop properly) and aberrant intraspetal vessels during open biopsy is currently the most reliable diagnostic indicator of atypical ACD/MPV. This represents an invaluable chance to differentiate living atypical patients from typical patients and increases the chance of appropriate treatment and improved prognosis for atypical ACD/MPV patients. Furthermore, the result from this study indicates that delayed onset of symptoms and longer survival can be associated with atypical ACD/MPV and that atypical ACD/MPV should always be considered/suspected when sudden onset of severe pulmonary hypertension presents in new-born infants. This research represents a crucial advancement in the understanding of a deadly and mysterious paediatric lung disease.
“Wang and Shi have unveiled abnormal cellular development features that may contribute to the development of congenital pulmonary airway malformation.”
CPAM: Common yet enigmatic lung lesion in children
In other research, Professors Wang and Shi have examined another lung condition that affects infants and young children: Congenital Pulmonary Airway Malformation (CPAM). CPAM is the most common congenital (present from birth) lesion (derived from the Latin ‘laesio’ for ‘injury’) found in the new-born lung. Approximately 25% of symptomatic patients will exhibit infection in the lungs and pneumothorax (the presence of air or gas in the cavity between the lungs and the chest wall, causing collapse of lung). However, 75% will be asymptomatic.
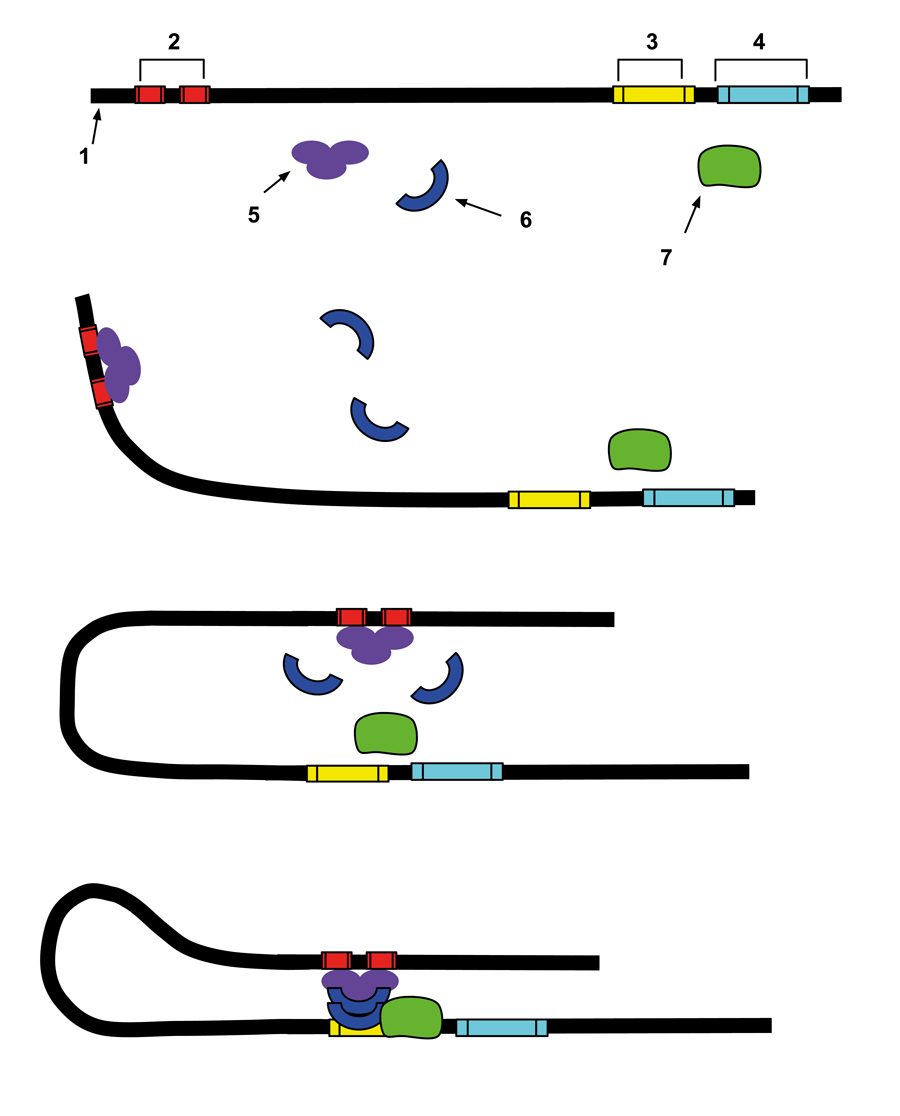
Types of CPAM
Five different types of CPAM exists, depending on where the lesion is presumably originated. Type 0 is characterised as a lesion in the trachea (windpipe), type 1; a lesion in the bronchi/ proximal bronchia, type 2; a lesion in the distal bronchia, type 3 a lesion in the bronchioalveolar region and type 4; a lesion in the acini. To aid in understanding of the locales of these lesions, it is helpful to consider the human lungs as analogous of a tree, with the trachea being the trunk, the right bronchus branching off into the right lung and the left bronchus into the left lung.
Type 1 and 2 are the most common types of CPAM. Many small cysts (<2cm in diameter) present in type 2 CPAM, whilst type 1 presents with larger cysts (>2cm diameter).
The mechanisms of disease development in CPAM remain enigmatic and no genetic factors have been identified associated with the development of CPAM. Incomplete understanding of the mechanisms of CPAM pathology are due in part to a lack of animal models that mimic the cellular environment and changes within the human lung when affected by CPAM.

Furthering the literature on CPAM
To help remedy this, Professors Wang and Shi have unveiled abnormal cellular developmental features that may contribute to the development of CPAM, such as the distinctive morphological changes that exist in the smooth muscle cells that line the airway. These cells are highly significant in the healthy development of foetal lungs. Smooth muscle around the bronchioles in healthy lungs are thick and have gaps between the bands. However, the researchers found that the smooth muscle layers around the airways of CPAM sufferers were significantly thinner and more frail. Additionally, the concentration of cilia (helpful hairlike structures that exist in the airways to keep the airways free of particulate matter) in the cystic cells were also seen to be significantly reduced. Furthermore, expression of elastin, a protein that is key in maintaining the extracellular matrix (the matrix of cells crucial to providing structural support to the cell) was drastically reduced in type 2 CPAM lungs compared to healthy lungs.
Infant mortality is a difficult topic that most would perhaps rather not contemplate. However, Professors Wang and Shi have taken up the mantle in furthering the literature on these under-researched pulmonary diseases, driving forwards progress to help improve infant/children morbidity and mortality associated with ACD/MPV and CPAM.

What is next for your research?
Based on our previous findings, we are going to move our research projects forward to better understanding the molecular and cellular mechanisms of these congenital lung disorders using state-of-the art technologies. In addition, we aim to translate our findings into clinical application to improve diagnosis and prognosis, and hopefully discover new treatment options for these pediatric patients suffering congenital lung disorders.
References
- Alturkustani, M. Li, D. Byers, J. Szymanski, L. Parham, D. Shi, W. Wang, L. (2021) Histopathologic features of alveolar capillary dysplasia with misalignment of pulmonary veins with atypical clinical presentation. Cardiovascular Pathology 50 1-6. https://doi.org/10.1016/j.carpath.2020.107289
- Jiang, Y. Luo, Y. Tang, Y. Moats, R. Warburton, D. Zhou, S. Lou, J. Pryhuber, G. Shi, W. Wang, L. (2019) Alternation of cystic airway mesenchyme in congenital pulmonary airway malformation. Scientific Reports 9:5296. 1-8. https://doi.org/10.1038/s41598-019-41777-y
10.26904/RF-137-1606526488
Research Objectives
The research of Larry Wang and Wei Shi helps to improve infant morbidity and mortality associated with paediatric pulmonary disorders.
Bio

Dr Larry Wang is a Professor of Clinical Pathology at the Keck School of Medicine of the University of Southern California. His research includes paediatric lung diseases, solid tumours and liver diseases. He has published more than 100 peer-reviewed publication and book chapters in these fields.

Dr Wei Shi is a Professor in the Department of Surgery at the Keck School of Medicine of University of Southern California. He has been studying lung development, injury repair, and pulmonary diseases for more than two decades with more than 100 peer-reviewed publications.
Contact
Children’s Hospital Los Angeles, and University of Southern California
4650 Sunset Blvd. Los Angeles, CA 90027, USA
E: Lawang@chla.usc.edu
E: Wshi@chla.usc.edu
T: +1 3233618672









