Each year, 300,000 people worldwide are born with sickle cell disease (SCD), a painful and debilitating genetic disorder of red blood cells. SCD is potentially fatal, responsible for 9% of all infant mortality in low-resource regions, but early diagnosis and prompt treatment can save lives. Until now, however, both diagnosis and therapy have relied upon expensive blood tests which can only be carried out by specialised staff in large, centralised laboratories.
The scourge of sickle cell
Red blood cells are the body’s delivery trucks, transporting oxygen to each and every cell of the body. The key component of red blood cells is haemoglobin, a chemical compound that combines with oxygen in the lungs and releases it again in all tissues of the body. In SCD, sufferers inherit two mutated copies of the haemoglobin gene, causing them to produce haemoglobin S instead of the normal haemoglobin A, and rendering their red blood cells sickle-shaped instead of the usual doughnut-shaped version. Carriers of SCD have one mutated and one normal copy of the haemoglobin gene, and do not show symptoms of the disease, but can pass it on to their children. SCD is most common in those of African, Mediterranean, South and Central American, Middle Eastern, Indian and Caribbean descent.
IMonitoring levels of the different haemoglobins in the bloodstream, before, during and after transfusion, is crucial to successful SCD therapy![]()

The most effective means of therapy for SCD, used in about 90% of cases, is transfusion with normal blood containing haemoglobin A. Repeated transfusions help both to reduce the proportion of haemoglobin S in the body and to prevent stroke, one of the most common and damaging complications of the disease. However, transfusion carries risks if too many blood cells are given. Therefore, monitoring the proportion of the different types of haemoglobin in the bloodstream, before, during and after transfusion, is crucial to successful SCD therapy. Currently, the only way to measure the haemoglobin composition of blood is to send samples away to centralised laboratories, which can take two or three days to deliver results. Thus, transfusion rates are frequently estimated based on outdated blood test results.
BioMedomics steps in
An obvious solution to the issues of high cost and long turnaround of blood testing that presently hinder diagnosis and treatment of SCD, is to develop low-cost, portable testing kits that provide immediate results at the patient bedside. This is where BioMedomics, Inc. (http://www.biomedomics.com/) steps in. The company is a world leader in designing unique, rapid tests for blood disorders. Established a decade ago, BioMedomics, Inc., based in North Carolina, combines the expertise of high level researchers in biology, biochemistry and biomedical engineering to develop advanced technologies for effective diagnostic testing applicable in both high- and low-resource regions.
In a remarkable improvement upon existing systems, Hemo SCAN-S delivers accurate measurements of relative haemoglobin levels within fifteen minutes![]()

The Hemo SCAN-S solution
Developed from BioMedomics ground-breaking qualitative test for diagnostic screening of newborn babies, Hemo SCAN-S uses antibodies (highly-sensitive immune-system proteins), which recognise the protein configuration of different types of haemoglobin and can report their relative proportions within as little as fifteen minutes.
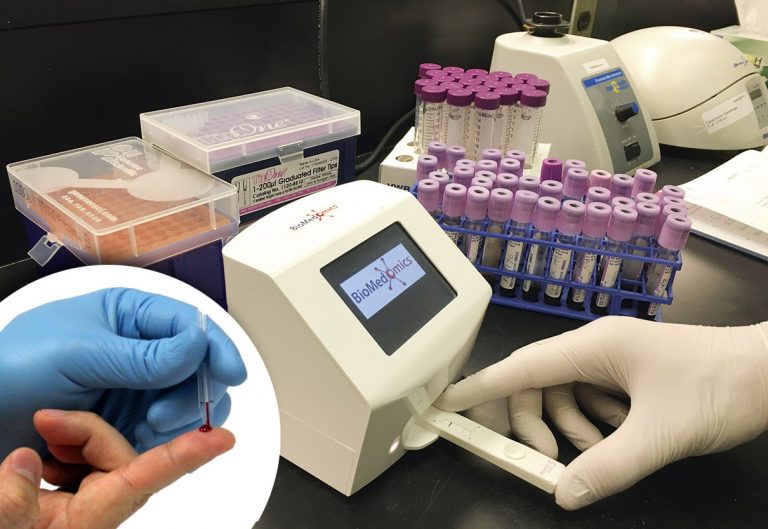
For SCD patients subjected to repetitive blood tests during treatment, it is important that testing be as simple and painless as possible; Hemo SCAN-S requires only a tiny drop of blood (five thousandths of a millilitre) which can be obtained by a simple finger-prick. The blood is placed onto a cartridge containing special chemicals which break down blood cells, releasing the haemoglobin contained therein. The haemoglobin then flows across a surface impregnated with the antibodies, which capture the different haemoglobin types and report their presence as coloured lines – much like the lines in a pregnancy test.
The truly exciting feature of the Hemo SCAN-S test is that the intensity of the lines is directly proportional to the concentration of the different types of haemoglobin present in the original blood sample. The intensity can be measured by a small, portable, red-light reader which reports results as easily-interpretable percentages. This enables transfusions to be matched precisely to the patient’s needs at the time of treatment.
Enhancing quality of life
BioMedomics have carried out extensive testing of the Hemo SCAN-S system and proven it to be highly sensitive to haemoglobin A and haemoglobin S, producing results as accurate and precise as those obtained in the traditional laboratory setting, and resistant to interference from other blood components. Compared to current central lab blood testing, Hemo SCAN-S completely eliminates the need to transport samples away from the patient bedside, thereby drastically reducing patient waiting time and potential over- or under-transfusion. In addition, the technology is simple to use, relatively painless, and of course rapid. For patients with SCD, Hemo SCAN-S – along with other diagnostic tools developed by the BioMedomics team – could revolutionise not just their treatment but their quality of life.
In SCD, mutated versions of the haemoglobin gene are inherited from both parents, causing red blood cells to become sickle shaped. These distorted cells die early causing anaemia or block the flow of blood causing severe pain crises. Damage caused by these rigid abnormal cells causes a potentially fatal stroke in a quarter of SCD children and adults by the age of 45. A life-long disease, SCD can negatively affect a person’s growth and harm organs such as spleen, brain, lungs, liver, kidneys, or skin.
How can transfusions help to mitigate the effects of SCD?
Blood transfusions limit the complications of SCD and consequently improve the life of an SCD patient. The rate of stroke can be reduced by more than 80% through the implementation of transfusion therapy. Transfusions can immediately alleviate aneamic conditions and also enhance quality of life for SCD patients with vital organ failure.
Why are current methods of blood testing inadequate?
Current methods used for monitoring transfusion therapy are haemoglobin fractionation in the central laboratory using haemoglobin electrophoresis, high performance liquid chromatography, or isoelectric focusing. These tests require a high equipment cost (>$100,000 USD), a trained technician to operate and maintain the system, and have turnaround times in the range of hours to days.
This breakthrough allows physicians to tailor transfusion therapy precisely to individual patient needs in real-time![]()
SCD patients requiring transfusions are guidelined to receive healthy HbA transfusions until their abnormal HbS levels reach <30% of total haemoglobin. Due to the long turnaround time of a haemoglobin fractionation test, the healthcare provider must estimate the amount of blood to transfuse using pretransfusion Hb concentration, body weight, and out-dated data from a previous visit. Missing the mark on the right amount of blood can have negative consequences and the burden of increased hospital visits. A patient may get an insufficient amount of healthy blood, and suffer painful, dangerous complications of SCD. Or, a patient may receive too much blood, and instead be faced with iron overdose.
How can a quantitative ‘point of care’ test help?
Our test system aims to produce patient data rapidly – while the clinician is with the patient. Rather than estimating the amount of blood to be applied to the patient using indirect clinical information, the healthcare provider can base decisions directly on the guidelined %HbS.
Accurate and current %HbS data would be available before, during, and after the transfusion to monitor the therapy. By applying the optimal amount of healthy blood, SCD patients can limit their disease complications, reduce the burden of hospital visits, and extend and improve their quality of life.
How could Hemo SCAN-S particularly benefit SCD patients in low-resource regions?
The easy-to-use Hemo SCAN-S test system (thousands of dollars) is several orders of magnitude less expensive than a central laboratory system (hundreds of thousands of dollars). The test system has a small desktop footprint and does not require a highly trained technician. Centres that provide transfusion therapy (US/Europe as well as in developing countries) could increase and improve usage of this life saving therapy through lower cost and ease-of-use.
BioMedomics, Inc. develops rapid, point-of-care diagnostic tools. Drs Jason Kim and Xiaoxi Yang have focused on creating a replacement test for relative haemoglobin levels to increase the accuracy of essential transfusion treatment for sickle cell disease sufferers.
Funding
North Carolina Biotechnology Center Small Business Loan Award; NIH Small Business Innovation Research Grants 1R43HL128670-01 and 2R44HL128670-02
Collaborators
Marilyn Telen, MD at Duke University Medical Center; Julie Kanter-Washko, MD at the Medical University of South Carolina; Russell Ware, MD at Cincinnati Children’s Hospital; Kwaku Ohene-Frempong, MD at the Sickle Cell Foundation of Ghana; Bishop and Church Leader Bob Kabugi of the Glorious Church of Kenya; Ampath Kenya
Bio
Jason S Kim, PhD is the Principal Investigator of both BioMedomics’ NIH NHLBI Small Business Innovation Research awards for point-of-care diagnostic tests for sickle cell disease. Dr Kim is the head of product development at BioMedomics, leading a team of talented engineers and scientists. Dr Kim previously held positions at Nanoentek Korea and the US Naval Research Laboratory in Washington DC.
Xiaoxi Yang is a co-PI of the NHLBI grants and director of research at BioMedomics. She was recruited based on her expertise and pedigree as a rising star in innovative sickle cell diagnostic research. Previously, Dr Yang held positions at the University of Houston and Tulane University.
Contact
Jason S Kim, PhD
BioMedomics, Inc.
Six Davis Drive,
Research Triangle Park, NC 27709
USA
E: jkim@biomedomics.com
T: +1 919 558 1210
W: www.biomedomics.com
www.sickle-scan.com
Twitter: @jason_biomedo
Facebook: /Biomedomics-Inc-521069534613488/