Scleroderma is a rare, autoimmune condition which causes the immune system to become overreactive and attack healthy body tissue. Its name derives from the Greek words ‘sclero’ for hard, and ‘derma’ for skin, as hardening of the skin due to an excess production of collagen tends to be one of the first noticeable symptoms associated with the condition. This extra collagen can also affect joints, tendons, and integral organs, preventing these parts of the body from functioning normally. Symptoms of scleroderma and their severity can vary from patient to patient, depending on the body parts affected by the disease. Generally, they include hardening of the skin, joint pain, stiffness, swelling of the hands and feet, and blood vessel damage. In some patients the internal organs, such as the heart, oesophagus, blood vessels, kidneys, lungs, and digestive system, are affected as much as the skin.
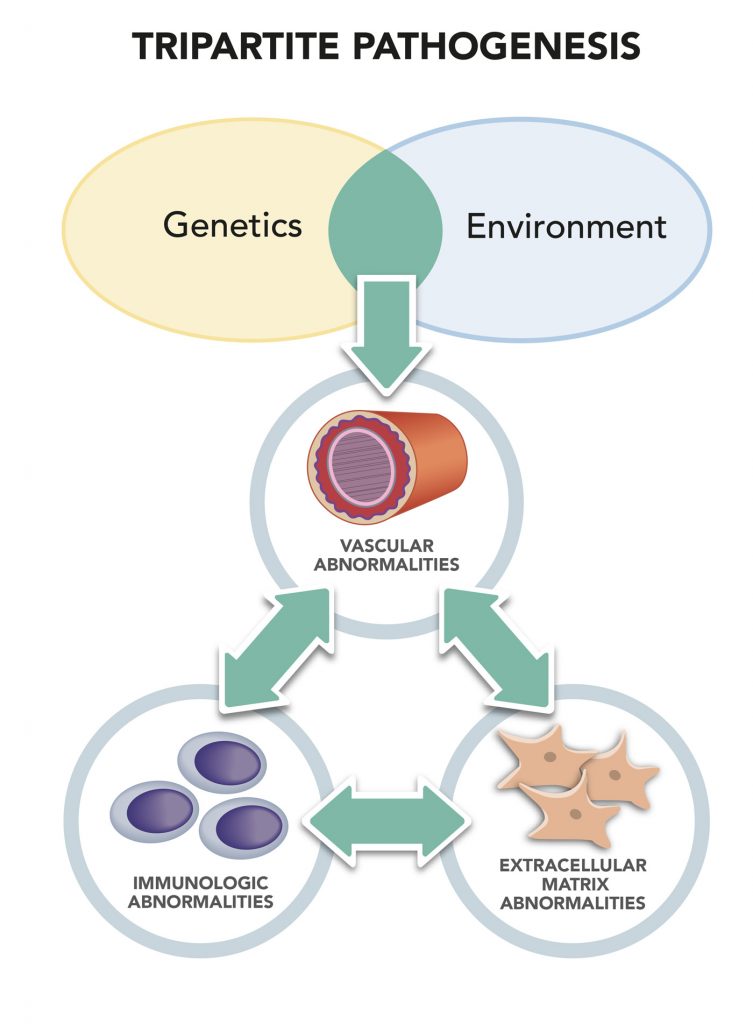
Vascular insufficiency tends to manifest itself in the early stages of scleroderma, with capillaries, the smallest blood vessels in the human body, deteriorating, despite evidence of an active repair process.
Biological underpinnings of fibrosis in scleroderma
Dr Trojanowska and her team have been carrying out extensive research exploring the biological underpinnings of both vascular disease and pathological fibrosis in scleroderma. They are trying to identify and characterise the key signalling pathways involved in the disease’s pathogenesis. Her laboratory’s studies are sponsored by the National Institute of Arthritis and Musculoskeletal and Skin Diseases (NIAMS), as well as the Scleroderma Foundation.
Fibrosis, a hallmark of scleroderma, is characterised by excessive deposition of collagen rich extracellular matrix in the skin and internal organs. In her initial work, Dr Trojanowska focused on the molecular mechanisms regulating excessive collagen production during fibrosis. These studies led to discovery of a potent transcription repressor of collagen: type I gene Friend leukaemia integration factor 1 (Fli1). This is an extremely important transcription factor that is expressed in the majority of cells. Further extensive studies in cultured skin fibroblasts demonstrated that the absence of Fli1 results in a large increase of collagen type I and other extracellular matrix genes. These findings were verified in human skin. In contrast to healthy skin in which the majority of fibroblasts produced Fli1, Fli1-positive fibroblasts were mainly absent from the skin of scleroderma patients with active disease. Fli1 protein expression was also significantly decreased in endothelial cells and other cells surrounding the small vessels in patient skin. More recent studies conducted in the laboratory of a collaborator, Dr Asano at Tokyo University, showed that in scleroderma patients, Fli1 is also diminished in keratinocytes, the cells that form the outer layer of the skin. Collectively, these studies point to a general deficiency of Fli1 in the skin of patients with scleroderma. Researchers don’t yet know why Fli1 is downregulated but this is another area Dr Trojanowska is investigating – it may be that epigenetic mechanisms, viruses or inflammation play a role.
Further studies carried out in mice that lack the Fli1 gene in endothelial cells showed that Fli1 has a critical role in the process of vessel maturation. This suggests that Fli1 deficiency plays a pathological role in microvascular disease of scleroderma, although it is still unclear whether these changes are specific to scleroderma or are also present in other vasculopathies. Remarkably, deficiency of Fli1 in keratinocytes impacted not only keratinocyte function, but also led to skin fibrosis and autoimmunity. Dr Trojanowska and her group have found links to Fli1 during another study, focusing this time on the lungs. Is it not until scleroderma spreads to the internal organs, particularly the lungs, that it becomes fatal. The researchers found deficiencies in the closest homolog of Fli1, ETS-related gene (ERG), and transcription factor GATA-6 in lung blood vessels to have a critical role in the development and disease progression of pulmonary arterial hypertension (PAH). This is a fatal condition of high blood pressure in the arteries transporting blood from the heart to the lungs present in some patients affected by scleroderma.
As there is currently no known cure for scleroderma, studies exploring the biological underpinnings of the disease are of crucial importance ![]()
Developing new therapies for pathological fibrosis
Dr Trojanowska and her team have successfully generated new genetic mouse models that sum up many of the vascular features of scleroderma. “Such models are instrumental in elucidating the mechanisms of vascular disease and for the discovery and validation of novel therapies to treat vasculopathy and fibrosis in patients with scleroderma,” explains Dr Trojanowska.
Dr Trojanowska’s research could also help to identify specific therapeutic agents that might alleviate and treat fibrosis in patients affected by scleroderma. For instance, her laboratory has been evaluating Dimethyl Fumarate (DMF, Tecfidera), an FDA-approved chemical agent with distinct anti-inflammatory and antioxidative properties. DMF and other fumarates have already shown promising results in treating several conditions, including psoriasis, alopecia, and multiple sclerosis. In pre-clinical scleroderma models, Dr Trojanowska found that DMF was effective in reversing PAH: reducing inflammation, oxidative damage, and lung fibrosis. These findings have led to a pilot trial of DMF for scleroderma-associated PAH, which is currently underway.
As there is currently no known cure for scleroderma, studies exploring the biological underpinnings of the disease are of crucial importance. “An improved knowledge of the molecular and cellular pathways that contribute to scleroderma vasculopathy could help in the design of effective therapies in the future,” reads one of Dr Trojanowska’s research papers.
Vascular disease contributes significantly to the severity of the illness and mortality of affected patients ![]()
Research carried out by Dr Trojanowska and her team has proved to be of substantial value, shedding light on some of the mechanisms behind vascular disease and identifying chemical agents that could help treat PAH and pathological fibrosis, present in some patients affected by scleroderma.
So far, Dr Trojanowska’s lab has collected important empirical evidence that links deficiencies in Fli1, ERG and GATA-6 protein with particular health conditions associated with scleroderma. Her work has also highlighted the potential of DMF to reverse PAH and lung fibrosis, leading to a pilot-trial that is currently evaluating its effectiveness on patients affected by scleroderma.
When I was recruited by Professor Carwile LeRoy, a leader in the scleroderma field, to contribute my expertise in molecular biology to help answer a fundamental question in scleroderma: what drives excessive production of collagen in scleroderma fibroblasts?
What do you feel have been your most meaningful findings so far and why?
Discovery of the connection between Fli1 gene and scleroderma. Scleroderma pathogenesis is very complex and despite the efforts of many scientists around the world, the factors that drive this disease are still not fully understood. I believe that the studies of Fli1 regulation and function have helped to clarify some aspects of scleroderma, but many questions still remain to be answered. We shared our Fli1 knockout mice with the investigators in the US and other countries and we expect to learn more about this gene in other organs or other diseases.
How could the mouse models devised by you and your team pave the way towards more effective treatments for vasculopathy and fibrosis in patients with scleroderma?
In our animal models we try to recapitulate the pathogenic processes occurring in patients with scleroderma. We already discussed deficiency of Fli1 in the skin, which prompted generation of mice with the cell type specific deletion ofFli1 gene. These models informed us about disease mechanisms and have already been used for drug testing. Similarly, we found that expression of GATA-6 and ERG is diminished in the lung vasculature of scleroderma patients with PAH and we are currently testing the therapeutic effects of dimethyl fumarate in these mice. Such studies may lead to discovery of potential biomarkers that may indicate a clinical response to DMF and could be utilised in clinical testing of DMF in scleroderma patients.
What are your plans for future investigation?
We are planning to take advantage of the new, cutting edge technologies, e.g. single cell RNA seq, to gain new insights into the abnormal characteristics of individual cells in the diseased tissues. This will allow us to understand more about the disease and potentially look at novel targets for the drug therapies.
Scleroderma pathogenesis is very complex and the factors that drive this disease are still not fully understood ![]()
Dr Trojanowska’s work focuses on scleroderma. She aims to understand the mechanism of pathological fibrosis in scleroderma.
Funding
Research in Dr Trojanowska’s lab is sponsored by the National Institute of Arthritis and Musculoskeletal and Skin Diseases (NIAMS) and the Scleroderma Foundation (http://www.scleroderma.org/site/PageServer#.WlaHI5M-e_o)
Collaborators
- Dr Robert Simms, Boston University
- Dr Robert Lafyatis, University of Pittsburgh
- Dr Yoshihide Asano, Tokyo University
Bio
 Dr Trojanowska earned her MS from Warsaw University and PhD from the Polish Academy of Sciences, Institute of Biochemistry and Biophysics in Warsaw. She began to study scleroderma in 1986, when she joined an internationally renowned Scleroderma Program directed by Professor Carwile LeRoy at the Medical University of South Carolina. In 2009 her laboratory was relocated to Boston, where she was appointed a Professor of Medicine and Director of the Arthritis Center at the Boston University School of Medicine.
Dr Trojanowska earned her MS from Warsaw University and PhD from the Polish Academy of Sciences, Institute of Biochemistry and Biophysics in Warsaw. She began to study scleroderma in 1986, when she joined an internationally renowned Scleroderma Program directed by Professor Carwile LeRoy at the Medical University of South Carolina. In 2009 her laboratory was relocated to Boston, where she was appointed a Professor of Medicine and Director of the Arthritis Center at the Boston University School of Medicine.
Contact
Maria Trojanowska, PhD
Alan S. Cohen Professor of Rheumatology
Director, Arthritis Center
Boston University School of Medicine
72 East Concord Street, E-5
Boston, Massachusetts 02118-2526
USA
E: trojanme@bu.edu
T: +1 617 638 4318
W: www.bu.edu/cort/key-personnel/maria-trojanowska-ph-d/